Venous Ulcers
LA Vascular Specialists
Vascular Specialists located in Beverly Hills, CA & Encino, CA
Venous ulcers are open sores that develop on the lower legs due to chronic venous insufficiency. This condition occurs when the valves in the leg veins do not function properly, causing blood to pool in the veins. Risk factors for venous ulcers include age, obesity, a history of deep vein thrombosis, and genetic factors.
Venous Ulcers: Diagnosis and Treatment
Diagnosing a venous ulcer involves a thorough physical examination. The characteristic findings include a shallow, irregularly shaped wound with a red or yellowish base, often surrounded by edema and hyperpigmentation. It may also present with signs of venous insufficiency, such as varicose veins and edema.
Treatment options for venous ulcers aim to improve venous circulation, promote wound healing, and prevent infection. Leg elevation is a simple and effective intervention that reduces edema and promotes blood flow. Compression therapy, using bandages or compression stockings, is key to providing external pressure and improving venous return. This helps to reduce edema, wound size, and recurrence rates.
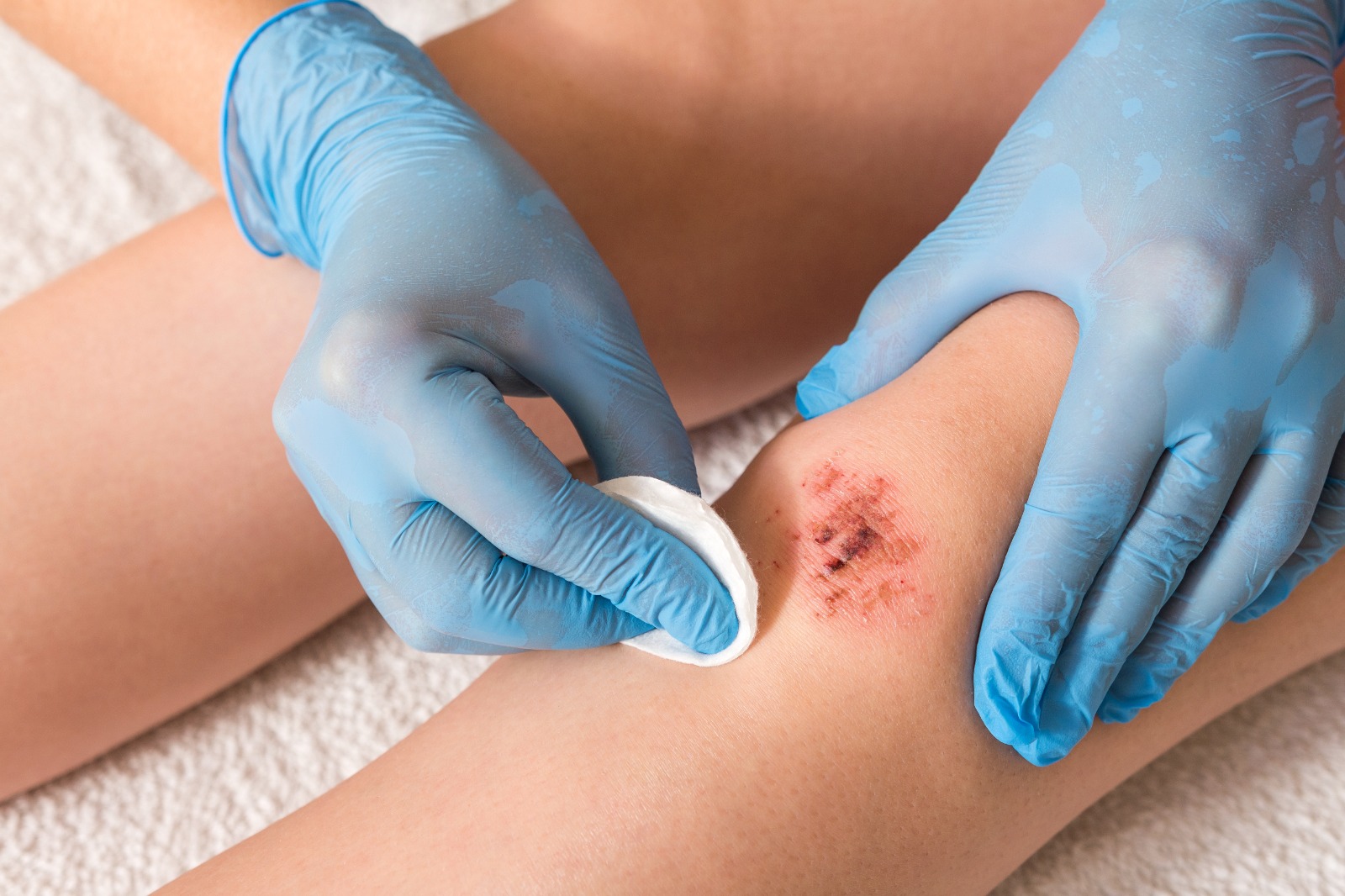
Evidence-based treatment options for venous ulcers also include the use of specialized dressings, such as hydrocolloids or foam dressings, which promote a moist wound environment and facilitate healing. Pentoxifylline, a medication that improves blood flow, may be prescribed to enhance wound healing. Aspirin therapy may also be considered to reduce inflammation and promote vascular health.
Venous ulcers can lead to complications such as cellulitis, osteomyelitis, and deep venous thrombosis. Prompt diagnosis and appropriate treatment are essential to prevent these complications and promote healing. Overall, a multi-faceted approach, including lifestyle modifications, wound care, and medical interventions, is crucial for successful management of venous ulcers.
Pathophysiology of Venous Ulcers
Venous ulcers, also known as stasis ulcers, are chronic wounds that occur as a result of impaired venous circulation. Venous insufficiency, the underlying cause of these ulcers, occurs when the valves in the veins become damaged or weakened, leading to backward flow of blood and increased pressure in the veins. This increased pressure causes fluid to leak out of the blood vessels and into the surrounding tissue, leading to tissue edema.
The impaired circulation seen in venous insufficiency results in poor oxygenation and nutrient delivery to the affected tissues, leading to tissue hypoxia and impaired wound healing. Additionally, the high pressure in the veins causes damage to the surrounding tissues and the small blood vessels, leading to localized inflammation and tissue damage.
Venous ulcers have specific characteristics that differentiate them from other types of ulcers. They typically occur in the lower extremities, usually around the ankles. The ulcers are typically shallow with irregular edges and a granulated, beefy red appearance. They tend to be painless unless complicated by infection.
Multiple factors contribute to the pathogenesis of venous ulcers. These include venous hypertension, impaired lymphatic drainage, and valve dysfunction. Venous hypertension leads to increased hydrostatic pressure, resulting in extravasation of fluid and protein into the interstitial space, causing tissue edema and inflammation. Impaired lymphatic drainage further exacerbates the edema and inflammation, while valve dysfunction allows for retrograde blood flow and pooling, worsening the venous hypertension.
Inflammation plays a significant role in the progression of venous ulcers. As the inflammatory response persists, it leads to further tissue damage, impaired wound healing, and dilation of blood vessels, causing perpetuation of the ulcerative process.
Overall, the pathophysiology of venous ulcers involves a complex interplay of venous insufficiency, impaired circulation, inflammation, and tissue damage. Understanding these underlying mechanisms is crucial for the effective management and treatment of venous ulcers.
Clinical Presentation and Diagnosis of Venous Ulcers
This section will discuss the clinical presentation and diagnosis of venous ulcers. Venous ulcers are a common type of chronic wound that can cause significant morbidity and impaired quality of life for affected individuals. Understanding the clinical features and appropriate diagnostic methods is crucial for accurate diagnosis and effective management of venous ulcers.
Common Lower Extremity Ulcers
Common lower extremity ulcers are a significant health concern that can cause considerable discomfort and impairment in affected individuals. These ulcers typically present with various characteristic features, such as a dull ache or pain, swelling, eczematous changes, and the presence of varicose veins. They are commonly found over bony prominences, especially in the gaiter area of the lower leg.
Upon physical examination, common lower extremity ulcers are typically observed as irregular and shallow wounds. These wounds often exhibit the presence of granulation tissue and fibrin, which are indicative of the healing process. Granulation tissue is characterized by the presence of small, fragile blood vessels that appear as a reddish-pink tissue. Fibrin, on the other hand, is a protein involved in clot formation and creates a yellowish layer over the wound.
The irregular nature of these ulcers is due to the underlying pathophysiology, which is usually influenced by conditions such as venous insufficiency, arterial disease, or a combination of both. Venous insufficiency can lead to chronic venous hypertension, resulting in impaired blood flow and subsequent tissue damage. Arterial disease, such as peripheral artery disease, can cause inadequate blood supply to the affected area, further contributing to ulcer formation.
In conclusion, common lower extremity ulcers are characterized by their dull ache or pain, swelling, eczematous changes, and the presence of varicose veins. Upon physical examination, these ulcers are irregular and shallow with the presence of granulation tissue and fibrin. Early recognition and appropriate management of these ulcers are crucial to prevent complications and promote healing.
Differential Diagnosis of Venous Ulcers
Venous ulcers are a common type of lower extremity ulceration that occurs due to chronic venous insufficiency. However, it is important to consider other possible etiologies when diagnosing and managing these ulcers. Differential diagnosis involves ruling out other potential causes of lower extremity ulcerations, including arterial insufficiency, prolonged pressure, diabetic neuropathy, systemic illnesses such as rheumatoid arthritis, vasculitis, osteomyelitis, and skin malignancy.
Arterial insufficiency is characterized by inadequate blood flow to the lower extremities, leading to tissue ischemia and ulcer formation. These ulcers are typically located on the distal aspects of the lower limbs, particularly near the toes. They are often painful, have a pale appearance, and may have associated signs of arterial disease such as decreased or absent pulses.
Prolonged pressure ulcers occur due to long periods of pressure on specific areas of the body, usually from immobility or prolonged wheelchair use. These ulcers commonly occur over bony prominences, such as the sacrum, heels, or elbows. They are often painful and may have a necrotic or eschar-covered appearance.
Diabetic neuropathy can lead to the development of foot ulcers in individuals with diabetes. These ulcers are typically located on the plantar surface of the foot, particularly the metatarsal heads. They are often painless due to sensory neuropathy and may have a callus rim and evidence of peripheral neuropathy.
In some cases, systemic illnesses such as rheumatoid arthritis and vasculitis can cause ulcerations in the lower extremities. These ulcers often present with other signs and symptoms of these underlying conditions, such as joint swelling, pain, or skin changes.
Other rare etiologies of lower extremity ulcerations include osteomyelitis and skin malignancy. Osteomyelitis is an infection of the bone that can result in the breakdown of soft tissues and the development of ulcers. Skin malignancies, such as squamous cell carcinoma or melanoma, can also present as non-healing ulcers that do not improve with traditional wound care.
In conclusion, the differential diagnosis of venous ulcers includes considering other potential etiologies such as arterial insufficiency, prolonged pressure ulcers, diabetic neuropathy, systemic illnesses like rheumatoid arthritis and vasculitis, osteomyelitis, and skin malignancy. It is crucial to carefully evaluate and differentiate these conditions to provide appropriate treatment and prevent complications.
Treatment of Venous Ulcers
Venous ulcers are a common and chronic condition that affects millions of people worldwide. These open sores typically occur on the lower legs and are caused by impaired blood flow in the veins, leading to the pooling of blood in the legs and subsequent tissue damage. Treating venous ulcers involves a multimodal approach that aims to alleviate symptoms, promote healing, and prevent recurrence. This includes addressing the underlying venous insufficiency, maintaining proper wound care, managing pain and inflammation, and implementing lifestyle changes to improve overall vascular health. In this article, we will explore the various treatment options available for venous ulcers and the importance of comprehensive management in achieving successful outcomes.
Debridement of Venous Ulcers
Debridement is a crucial procedure utilized in the treatment of venous ulcers, which involves the removal of dead tissue from the wound. It plays a vital role in promoting healing and preventing infection.
The process of debridement serves to eliminate necrotic tissue, slough, and any devitalized material present in the wound. This dead tissue is a breeding ground for bacteria, hindering the healing process and increasing the risk of infection. By removing this non-viable tissue, debridement promotes a clean wound bed, facilitating the growth of healthy granulation tissue.
The importance of debridement in promoting healing lies in its ability to stimulate the formation of new blood vessels, allowing increased oxygen and nutrient delivery to the wound area. Additionally, this procedure also aids in the removal of biofilm, which can be a barrier to effective wound healing.
There are various methods of debridement that can be employed. Surgical debridement involves the use of instruments like scalpels or scissors to physically cut away the dead tissue. This method is effective for large amounts of necrotic tissue. On the other hand, enzymatic debridement utilizes topical agents such as collagenase or proteolytic enzymes to dissolve and break down the necrotic tissue. Other methods include autolytic debridement, which utilizes the body's natural enzymes to dissolve dead tissue, and mechanical debridement, which involves the use of forces like dressings or pulsatile irrigation to physically remove necrotic material.
To conclude, debridement is a critical process in the management of venous ulcers. By effectively removing dead tissue, it not only promotes healing but also prevents infection. Different methods of debridement can be utilized based on the specific requirements of the individual case, assisting in the restoration of healthy tissue and facilitating wound closure.
Compression Therapy
Compression therapy is a medical treatment that aims to reduce edema and pain, improve venous reflux, and enhance the healing process of venous ulcers. This therapy involves the application of external pressure to the affected area, compressing the underlying tissue and aiding in the management of various conditions.
There are several different types of compression therapy that can be utilized based on the specific needs of the patient. Elastic bandages, also known as elastic compression bandages, are commonly used and are designed to stretch and adapt to the contours of the body. They provide consistent pressure and support, helping to reduce swelling and promote blood flow. Elastic bandages are often used in the initial management of acute injuries and are also effective in the long-term treatment of venous ulcers.
In addition to elastic bandages, inelastic wraps are another form of compression therapy. Unlike elastic bandages, inelastic wraps do not stretch, providing more rigid compression to the affected area. These wraps are often used to treat chronic venous insufficiency and can provide greater compression for patients with more advanced conditions.
Compression stockings are another commonly used form of compression therapy. These stockings apply graduated pressure along the leg, with the highest pressure at the ankle and gradually decreasing up the leg. They are specifically designed to improve venous return and prevent pooling of blood in the lower limbs. Compression stockings are often recommended for individuals who are at risk for developing deep vein thrombosis, such as those who have recently undergone surgery or have prolonged periods of inactivity.
Lastly, intermittent pneumatic compression (IPC) devices are a type of compression therapy that involves the use of an air pump and inflatable sleeves. These devices apply intermittent pressure to the affected area, mimicking the natural pumping action of the muscles and promoting venous return. IPC devices are often used in the management of deep vein thrombosis, lymphedema, and other conditions that require increased blood flow and drainage.
In conclusion, compression therapy is a versatile and effective treatment option for a variety of conditions. Whether it be through the use of elastic bandages, inelastic wraps, compression stockings, or intermittent pneumatic compression devices, compression therapy can provide significant benefits in reducing edema, improving venous reflux, and enhancing the healing process of venous ulcers.
Leg Elevation
Leg elevation is a crucial component of standard care when paired with compression therapy for various lower limb conditions. The benefits of leg elevation are numerous and can greatly contribute to a patient's overall healing and well-being.
One of the key advantages of leg elevation is its ability to reduce edema. Elevating the legs helps to facilitate the return of blood and fluid flow from the lower extremities back towards the heart. This helps to alleviate swelling and decrease the accumulation of excess fluid in the legs. By reducing edema, the risk of complications such as skin breakdown and infection is also mitigated.
In addition to reducing edema, leg elevation improves microcirculation. By raising the legs above heart level, blood flow is enhanced, allowing for better distribution of oxygen and nutrients to the surrounding tissues. This enhanced microcirculation promotes healing and can accelerate the recovery process.
Leg elevation also plays a vital role in hastening ulcer healing. Ulcers, particularly those associated with conditions like venous insufficiency or peripheral arterial disease, require effective blood flow for proper healing. Leg elevation aids in decreasing pressure in the ulcerated area, allowing for improved blood flow and enhanced wound healing.
The recommended duration and frequency of leg elevation may vary based on the specific condition and severity. However, it is generally advised to elevate the legs for at least 30 minutes, 3 to 4 times a day. Persistent adherence to this routine is crucial for achieving optimal benefits. However, patients may face challenges in adhering to this treatment, such as discomfort, inconvenience, or mobility limitations. Health care professionals must work with patients to address these challenges and develop individualized strategies to ensure compliance.
In conclusion, leg elevation is a vital component of care when combined with compression therapy. Its importance lies in reducing edema, improving microcirculation, and hastening ulcer healing. While there may be challenges in adhering to leg elevation, diligent and consistent implementation of this treatment can greatly contribute to a patient's overall improvement and well-being.
Exercise
The systematic review mentioned in the Background Information aimed to investigate the effectiveness of different exercises for venous ulcers. The review analyzed various studies and found that exercise can significantly contribute to the healing of venous ulcers.
Specifically, the review highlighted the impact of progressive resistance exercise when combined with prescribed physical activity. Progressive resistance exercise is a type of exercise that involves gradually increasing the resistance or load to improve muscle strength and function. The prescribed physical activity refers to a structured exercise program specifically designed for individuals with venous ulcers.
The review suggested that progressive resistance exercise with prescribed physical activity demonstrated superior healing outcomes compared to other types of exercises. This combination of exercises promotes the development of muscle strength and function, leading to increased blood flow and improved healing of venous ulcers.
By incorporating progressive resistance exercise and prescribed physical activity into the treatment plan for venous ulcers, healthcare practitioners can effectively enhance the healing process. This approach helps to address the underlying issues associated with venous insufficiency and improve overall patient outcomes.
In conclusion, based on the systematic review, progressive resistance exercise with prescribed physical activity has shown to be effective in promoting the healing of venous ulcers. Implementing this type of exercise regimen can significantly contribute to improved outcomes for individuals with venous ulcers.
Dressings
There are several types of dressings commonly used under compression bandages to promote faster healing and prevent adherence of the bandage to the ulcer. These dressings serve to create a moist environment, facilitate wound debridement, enhance cellular migration, and provide protection against microorganisms. Some of the commonly used dressings include:
1. Foam dressings: These dressings are highly absorbent and provide excellent cushioning and protection. They help maintain a moist wound environment and promote granulation tissue formation.
2. Hydrogel dressings: These dressings contain a high percentage of water and are ideal for dry or necrotic wounds. They provide hydration to the wound bed and promote autolytic debridement.
3. Alginate dressings: These dressings are made from seaweed and are highly absorbent. They are particularly useful for wounds with high exudate levels. Alginate dressings form a gel-like substance when they come into contact with wound fluid, which helps facilitate the removal of necrotic tissue.
4. Hydrocolloid dressings: These dressings contain gel-forming agents and provide a moist environment for wound healing. They are impermeable to bacteria and offer protection against contamination.
5. Transparent films: These dressings are topically applied and are ideal for superficial wounds or as a secondary dressing. They allow the visualization of the wound and provide a moisture barrier.
While there are various types of dressings used under compression bandages, a meta-analysis of 42 randomized controlled trials concluded that there was no significant difference among dressing types in terms of promoting faster healing and preventing adherence of the bandage to the ulcer. Therefore, the choice of dressing should be based on factors such as wound characteristics, exudate levels, and patient preference.
Types of Dressings Used for Venous Ulcers
Venous ulcers are a common complication of chronic venous insufficiency and can be challenging to manage. Dressings play a crucial role in promoting wound healing and preventing infection. There are several types of dressings available for venous ulcers, each with its own unique properties.
Topical antiseptics are commonly used to cleanse the wound and reduce bacterial load. Some examples include cadexomer iodine, povidone-iodine, peroxide-based preparations, honey-based preparations, and silver dressings. These antiseptics help in reducing wound exudate, promoting granulation tissue formation, and controlling infection.
Medications can be utilized to aid wound healing and reduce inflammation. Pentoxifylline, a drug that improves blood flow, has shown promising results in treating venous ulcers. Statins and phlebotonics, such as horse chestnut extract, can also be beneficial in improving venous circulation. Antibiotics may be prescribed in cases where infection is suspected or confirmed.
Advanced therapies, including cellular and tissue-based products, and skin grafting, are reserved for more severe and chronic ulcers that fail to heal with conventional treatments. These therapies promote wound bed preparation, angiogenesis, and cellular regeneration.
Endovenous interventions are targeted at addressing the underlying venous insufficiency contributing to ulcer development. These procedures, including endovenous ablation, ligation, subfascial endoscopic perforator surgery, and sclerotherapy, aim to improve venous return and reduce ulcer recurrence.
In conclusion, the management of venous ulcers requires a multimodal approach. The choice of dressing depends on the characteristics of the wound and the patient's specific needs. Topical antiseptics, medications, advanced therapies, and endovenous interventions all play a crucial role in the treatment of venous ulcers.
Medications
Venous ulcers are chronic wounds that result from poor venous circulation, leading to increased levels of inflammation, tissue damage, and impaired healing. Several medications can be used for the treatment of venous ulcers, including pentoxifylline, statins, phlebotonics, antibiotics, and hyperbaric oxygen therapy.
Pentoxifylline is a medication that improves blood flow by reducing blood viscosity and increasing red blood cell flexibility. It also has anti-inflammatory properties, which can reduce inflammation associated with venous ulcers. Studies have shown that pentoxifylline can improve wound healing and promote ulcer closure.
Statins, commonly used to manage high cholesterol levels, have also been found to have potential benefits in the treatment of venous ulcers. Statins can improve endothelial function, promote tissue repair, and modulate inflammatory processes, which may help in the healing of venous ulcers.
Phlebotonics, including flavonoids and micronized purified flavonoid fraction (MPFF), are medications that strengthen blood vessel walls, reduce venous inflammation, and improve overall venous circulation. These medications have shown positive effects in reducing pain, edema, and promoting ulcer healing in patients with venous ulcers.
In some cases, venous ulcers may become infected, requiring the use of antibiotics. Antibiotics are prescribed to control and eliminate bacterial infections, preventing further complications. The choice of antibiotic may vary depending on the type and severity of the infection.
Hyperbaric oxygen therapy (HBOT) involves breathing pure oxygen in a pressurized chamber, which promotes increased oxygen levels in the blood and accelerates wound healing. HBOT can be beneficial for the treatment of non-healing venous ulcers, as it promotes tissue repair and regeneration.
It is important to consult with a healthcare professional for a thorough evaluation and to determine the most appropriate medication(s) for the treatment of venous ulcers, as individual patient factors and the severity of the ulcer may influence medication choices.
Advanced Therapies
Advanced therapies have emerged as effective options for the treatment of refractory venous ulcers. These therapies include cellular and tissue-based products (CTPs) and skin grafting, both of which have been shown to shorten healing time and improve healing rates when compared to the traditional approach of compression plus a simple dressing.
Cellular and tissue-based products are derived from human or animal cells and are designed to promote tissue regeneration. They provide a rich source of growth factors, cytokines, and other bioactive molecules that stimulate the healing process. These products, such as platelet-rich plasma and human dermal fibroblast, can be applied directly to the wound bed. They have been found to accelerate healing by promoting angiogenesis, reducing inflammation, and enhancing cell proliferation.
Skin grafting involves taking a thin piece of healthy skin from one part of the body and transplanting it onto the ulcerated area. This procedure provides a new source of healthy cells that can replace the damaged tissue. Skin grafts can be particularly effective for large or non-healing venous ulcers as they provide a physical barrier to infection and aid in wound closure.
Both cellular and tissue-based products and skin grafting have been shown to significantly reduce healing time and improve healing rates compared to compression plus a simple dressing alone. These advanced therapies address the underlying causes of refractory venous ulcers and provide additional support for the natural healing process. By targeting specific aspects of wound healing, these therapies offer a more comprehensive and accelerated approach to ulcer treatment.
Endovenous Intervention
Endovenous interventions play a crucial role in the management of venous ulcers. These interventions include endovenous ablation, ligation, subfascial endoscopic perforator surgery (SEPS), and sclerotherapy.
Endovenous ablation is a minimally invasive procedure that uses laser or radiofrequency energy to close the affected veins. By sealing off these veins, blood flow is redirected to healthier veins, reducing the pooling of blood and pressure on the ulcer. This promotes healing and prevents further deterioration.
Ligation involves the surgical tying off of the problematic veins. This helps to stop the reverse flow of blood and reduce venous reflux, thus preventing the development and recurrence of ulcers.
SEPS is a procedure that aims to remove or repair the malfunctioning perforator veins, which are responsible for the ulcer formation. By correcting the underlying cause, this intervention helps to improve healing and prevent the recurrence of venous ulcers.
Sclerotherapy is a method that involves injecting a solution into the affected vein, causing it to collapse and close. This intervention improves blood flow and reduces the symptoms associated with venous ulcers. It is often used in combination with other endovenous interventions to achieve optimal outcomes.
Overall, these endovenous interventions aim to improve healing and prevent ulcer recurrence by addressing the underlying venous insufficiency. They facilitate blood flow redirection, reduce pooling of blood, repair malfunctioning veins, and close off problematic vessels. By effectively treating the root cause of venous ulcers, these interventions play a crucial role in the management and long-term prevention of this chronic condition.
Prevention of Recurrence of Venous Ulcers
Venous ulcers are a common and recurring problem for individuals with underlying venous insufficiency. To prevent the recurrence of venous ulcers, several preventive measures can be implemented.
First and foremost, it is essential to maintain the treatments for chronic conditions such as high blood pressure. Chronic conditions can be contributing factors to the development and recurrence of venous ulcers. Treating and managing these conditions effectively will reduce the likelihood of ulcers reoccurring.
Quitting smoking is another crucial step in preventing the recurrence of venous ulcers. Smoking impairs the blood flow and damages blood vessels, which can worsen venous insufficiency and increase the risk of ulceration. Therefore, individuals who smoke should quit to enhance their overall vascular health.
Furthermore, following medical instructions regarding the use of blood thinners is paramount for preventing the recurrence of venous ulcers. These medications help to reduce the risk of blood clots and improve circulation, thereby decreasing the chances of developing ulcers.
In addition to these measures, wearing compression stockings is highly recommended. Compression stockings improve venous return and help to prevent the formation of blood clots. They also aid in reducing swelling and promoting healthy blood flow in the legs.
Maintaining a healthy weight is another important strategy in preventing the recurrence of venous ulcers. Excess weight puts additional pressure on the veins, making it harder for blood to circulate properly. Losing weight can alleviate this burden and reduce the risk of ulcers forming.
Lastly, practicing proper skin care is crucial. Regularly moisturizing the skin and keeping it clean can help prevent dryness, cracking, and subsequent skin breakdown, which may lead to the development of ulcers.
In conclusion, preventing the recurrence of venous ulcers involves a combination of preventive measures such as quitting smoking, using blood thinners as prescribed, wearing compression stockings, losing weight, maintaining proper skin care, and managing chronic conditions like high blood pressure. By implementing these strategies, individuals can significantly reduce the likelihood of venous ulcers recurring and improve their overall vascular health.
Conclusion: Venous Ulcers
In conclusion, treatment options for venous skin ulcers involve various methods to improve blood circulation and promote healing. Elevating the legs above heart level and wearing compression stockings have proven effective in enhancing blood flow and reducing swelling in the affected area. These measures help alleviate symptoms and encourage the healing process.
Debridement, the process of removing dead tissue from the wound, is vital in the treatment of venous ulcers. It helps create a clean and healthy base for new tissue growth. Regular debridement ensures that the wound heals properly and reduces the risk of infection.
It is important to continue using compression therapy even after the ulcer has healed. Compression stockings help maintain proper blood flow, prevent the recurrence of ulcers, and minimize the risk of developing new ones. They provide support to the veins and improve overall circulation, thus promoting healthy skin.
If the ulcer fails to heal with the aforementioned methods, additional treatments may be required. These may include the use of antibiotics to treat any underlying infection, skin grafting to promote healing, or vein surgery to address any underlying venous insufficiency. These approaches aim to tackle the root cause of the ulcer and facilitate the healing process.
In summary, treatment options for venous skin ulcers involve improving blood circulation through methods such as leg elevation and compression stocking use. Debridement is crucial to remove dead tissue and promote healing. Continuing compression therapy post-healing is vital to prevent the recurrence of ulcers. In cases where ulcers do not heal, additional treatments such as antibiotics, skin grafting, or vein surgery may be necessary.
